
1/15/2020
PITTSBURGH – A study involving tens of thousands of bariatric surgery patients found that gastric bypass patients were significantly more likely than gastric sleeve patients to end up back in the hospital in the years following surgery.
The paper, published today in JAMA Surgery, describes one of the largest bariatric surgery studies ever done, and the first study of its size to focus on health problems years after the procedure.
 “In bariatric surgery, there has been an explosion of data, but most focuses on positive outcomes,” said lead author Anita Courcoulas, M.D., M.P.H., professor of surgery, University of Pittsburgh School of Medicine, and chief of minimally invasive bariatric surgery, UPMC. “This study is important because it includes adverse events people might be concerned about.”
“In bariatric surgery, there has been an explosion of data, but most focuses on positive outcomes,” said lead author Anita Courcoulas, M.D., M.P.H., professor of surgery, University of Pittsburgh School of Medicine, and chief of minimally invasive bariatric surgery, UPMC. “This study is important because it includes adverse events people might be concerned about.”
Drawing from data collected for the PCORnet Bariatric Study, the researchers examined electronic medical records from 33,560 bariatric surgery patients across 10 different medical centers from 2005-2015.
“It was critical to have so many sites participating because that helps make sure that our findings are relevant to patients from all around the country,” said coauthor David Arterburn, M.D., M.P.H., senior investigator, Kaiser Permanente Washington, and co-principal investigator of the PCORnet Bariatric Study.
About half of the patients included in this study underwent Roux-en-Y gastric bypass and the other half had sleeve gastrectomy.
With gastric sleeve surgery, the doctor treats obesity by removing a portion of the stomach so that patients eat less and feel full faster. With gastric bypass, the surgeon creates a stomach-like pouch in the intestine and short-circuits the stomach entirely, achieving the same effect.
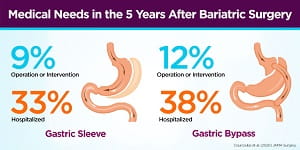 Five years after surgery, significantly more of the gastric bypass patients included in the study had undergone another abdominal operation or intervention, with an average of 12% of patients compared to 9% of those with a gastric sleeve. Endoscopy and hospitalization rates also were significantly higher for the gastric bypass group. There was no difference in mortality between the two groups after five years.
Five years after surgery, significantly more of the gastric bypass patients included in the study had undergone another abdominal operation or intervention, with an average of 12% of patients compared to 9% of those with a gastric sleeve. Endoscopy and hospitalization rates also were significantly higher for the gastric bypass group. There was no difference in mortality between the two groups after five years.
Courcoulas suspects the reason patients need more care in the years after gastric bypass is that it’s a more complex surgery than sleeve gastrectomy, though she was quick to point out that procedures for positive health changes, such as hernia repair, also were included in the analysis.
Although the risks seem slightly higher with gastric bypass, the potential benefits are greater, too. An earlier paper using the same PCORnet dataset showed that gastric bypass resulted in significantly more weight loss than gastric sleeve.
Ultimately, the results of these studies could be used to help patients and health care providers make more informed decisions about the type of bariatric surgery to pursue.
“What we advocate is high-quality shared decision making between providers and patients,” Courcoulas said. “It starts with a conversation about what their preferences and values are. Some people value low risk, some value high weight loss. It’s important to have information on both sides of the risk-benefit equation.”
Additional authors on the study include R. Yates Coley, Ph.D., Robert Wellman, M.S., Jane Anau and Andrea Cook, Ph.D., of Kaiser Permanente Washington; Jeanne Clark, M.D., of Johns Hopkins University; Corrigan McBride, M.D., of University of Nebraska Medical Center; Elizabeth Cirelli, M.S.N., and Ali Tavakkoli, M.D., of Brigham and Women’s Hospital; Kathleen McTigue, M.D., of Pitt; Karen Coleman, Ph.D., of Kaiser Permanente Southern California; Sengwee Toh, Ph.D., Jessica Sturtevant, M.S., and Casie Horgan, M.P.H., of Harvard Medical School and Harvard Pilgrim Health Care Institute; Cheri Janning, M.S., of Duke Clinical and Translational Science Institute; and Neely Williams, M.Div., of Community Partners’ Network.
This research was funded by the Patient-Centered Outcomes Research Institute (OBS-1505-30683).
MULTIMEDIA INFO: (click images for high-res versions)
CREDIT BOTH: UPMC
TOP: Anita Courcoulas, M.D., M.P.H.
BOTTOM: Infographic summarizing the main results of Courcoulas et al. (2020) JAMA Surgery.
















