An abdominal aortic aneurysm is a bulge that happens in a weak area of your aorta, affecting the portion that is located in your abdomen.
At UPMC, our vascular surgeons are experts in treating abdominal aortic aneurysms using minimally invasive repair techniques, depending on the severity of your condition. We take a team approach to quickly and accurately diagnose your condition and develop a treatment plan that's right for you.
On this page:
What Is An Abdominal Aortic Aneurysm?
The aorta is the main blood vessel in the body, supplying blood to the head, arms, legs, and organs in the chest and abdomen. An abdominal aortic aneurysm occurs when the aorta in the abdomen becomes abnormally large or balloons outward, causing a bulge.
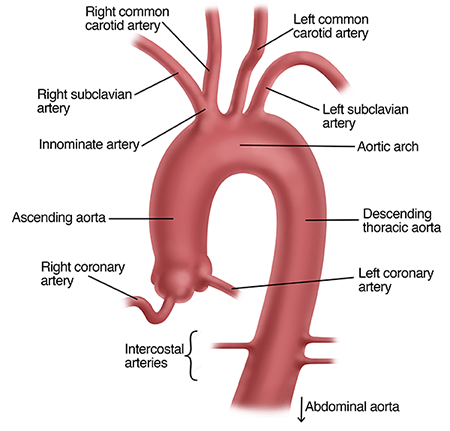
Although this can happen to almost any artery in the body, it is most common in the segment of the aorta located around the kidney arteries and before the aorta branches into the arteries leading to the legs.
How common is an abdominal aortic aneurysm?
Abdominal aortic aneurysms affect more than 1 percent of people over age 50. Although an aneurysm can happen to almost any artery in the body, it is most common in the segment of the aorta located around the kidney arteries and before the aorta branches into the arteries leading to the legs.
What causes abdominal aortic aneurysm?
Abdominal aortic aneurysms can develop in anyone, but the condition is often inherited. People with a family history of abdominal aortic aneurysm may be more likely to develop one themselves.
What are abdominal aortic aneurysm risk factors?
Abdominal aortic aneurysms are most often diagnosed in men over the age of 60, but anyone who has smoked tobacco is at risk of developing an aneurysm.
In addition to a family history of aortic aneurysms, additional factors that increase your risk include:
- Atherosclerosis, or hardening of the arteries.
- Connective tissue diseases, such as Marfan or Ehlers-Danlos syndrome.
- High blood pressure.
- High cholesterol.
- Smoking.
Complications of abdominal aortic aneurysm
Abdominal aortic aneurysms can cause serious complications if they burst or rupture. The larger the aneurysm, the more likely it is to rupture.
Ruptured aneurysms can result in life-threatening internal bleeding if not treated immediately. For this reason, early diagnosis of abdominal aortic aneurysms and regular appointments with your surgeon to track the growth of the aneurysm are important.
If the aneurysm is large or growing quickly, having elective surgery to repair it can prevent rupture in the future.
How can I prevent abdominal aortic aneurysm?
You may not be able to control some of your abdominal aortic aneurysm risk factors. However, preventing heart disease and chronic conditions can reduce the risk that you will develop an abdominal aortic aneurysm.
You may be able to reduce your risk by:
- Eating a diet that is rich in fruits, vegetables, and whole grains.
- Exercising and maintaining a healthy weight.
- Maintaining normal blood pressure and cholesterol levels.
- Avoiding smoking.
- Limiting alcoholic beverages.
What Are the Signs and Symptoms of Abdominal Aortic Aneurysm?
Aneurysms develop slowly over many years.
Most people do not feel any symptoms at all. Instead, most aneurysms are discovered either by a screening test ordered by a primary care doctor or on an imaging study such as an x-ray or CT scan done for another reason. Regardless of how it is diagnosed, an abdominal aortic aneurysm requires a follow-up appointment at least every 6-12 months to track its growth.
Are there early warning signs of an aortic aneurysm?
If symptoms do occur, this can be a sign that the aneurysm is about to rupture. Most people will have severe pain in their abdomen or back that comes on suddenly, and they may also feel dizzy, weak, or pass out.
When should I see a doctor about my abdominal aortic aneurysm symptoms?
If you are having symptoms caused by your abdominal aortic aneurysm, it may be a sign of a life-threatening situation that requires immediate medical care. You should dial 911 or go to the nearest hospital emergency room. A ruptured abdominal aortic aneurysm is a medical emergency with a high risk of death if not treated immediately.
How Do You Diagnose Abdominal Aortic Aneurysm?
If you are at high risk of developing an abdominal aortic aneurysm or if your doctor suspects one, you'll need to undergo a thorough physical exam.
What to expect during your visit
During your physical exam, your doctor will:
- Perform a screening.
- Ask you about your condition and symptoms.
- Examine your abdomen.
- Check the pulses in your legs.
Tests to diagnose abdominal aortic aneurysm
Following your exam, your doctor may order additional tests and procedures to help confirm the aneurysm and determine its size.
The care team at UPMC uses advanced imaging tests to help diagnose an abdominal aortic aneurysm, including:
- Computed tomography (CT) scan – This test uses a ring of multiple x-rays to create detailed 3D images of your aorta.
- Duplex ultrasound scanning – This painless test uses ultrasound waves to create images of the aneurysm.
- Magnetic resonance imaging (MRI) – MRI uses a large magnetic field, radio waves, and computers to create detailed images of your aorta.
Abdominal aortic aneurysm prognosis
Less than 50 percent of people survive a ruptured abdominal aortic aneurysm, so prevention is by far the best way to treat this condition.
Can abdominal aortic aneurysm be cured?
When an abdominal aortic aneurysm is diagnosed early, expert monitoring and treatment can reduce your risk of a life-threatening rupture and improve your overall prognosis.
How Do You Treat Abdominal Aortic Aneurysm?
The main treatment goal for an aortic aneurysm is early diagnosis in order to prevent rupture. UPMC offers a full range of state-of-the-art treatments for abdominal aortic aneurysms.
We create a customized treatment plan, which includes an assessment of:
- The location of the aneurysm and the severity of your condition.
- The size of the aneurysm.
- Your overall health, including a focused evaluation of your heart, kidneys, and lungs.
Based on our findings, we may recommend one of the following treatment options:
Treatment for small aneurysms (less than 2 inches in diameter)
Treatment for small aneurysms may include:
- Duplex ultrasound scan every 6-12 months to assess the aneurysm's size.
- Lifestyle changes, such as quitting smoking.
- Medication to lower your blood pressure if your blood pressure is high.
- Medication to lower your cholesterol and reduce inflammation.
- Regular follow-up visits to closely monitor the abdominal aortic aneurysm.
Treatment for large aneurysms (greater than 2 inches in diameter)
At this size, the risk of rupture is still low, but the risk will rapidly increase if the aneurysm continues to grow. Surgery is often recommended and may be either minimally invasive or traditional to repair the aneurysm before it ruptures.
Surgery for abdominal aortic aneurysm
Aneurysm treatment aims to replace the aorta with a man-made graft. This redirects the blood flow through the graft and away from the weakened aneurysm wall, preventing the aneurysm from getting bigger or rupturing. After the repair, the aneurysm will usually shrink over time.
Our experts are able to offer the widest variety of surgical treatments ranging from traditional surgery to the most complex minimally invasive techniques available. The main treatments for abdominal aortic aneurysms include:
- Minimally invasive endovascular aneurysm repair (EVAR).
- Traditional (open) surgery.
- “Hybrid" procedures that combine open surgery, surgical repair, and minimally invasive techniques.
Our surgeons typically advise surgery when:
- The aneurysm reaches approximately five centimeters (about two inches) in diameter.
- Smaller aneurysms exist that cause symptoms or grow rapidly.
These are general guidelines, and each patient is different. Your vascular surgeon will discuss your individual risks and benefits of surgery and decide with you whether to wait or undergo a repair.
Endovascular aneurysm repair (EVAR)
The majority of abdominal aortic aneurysms can be repaired with a minimally invasive EVAR procedure. Whether or not you can receive an EVAR depends on the aneurysm's shape, location, and extent.
In contrast to a traditional “open" surgery, no big incisions are made in the abdomen. Instead, the arteries in the groin are accessed either by a needle puncture or a small incision.
During EVAR, your doctor will:
- Insert a small, thin tube called a catheter through a small incision into a blood vessel in your groin.
- Use a catheter to guide a small metal and fabric tube called a stent through your blood vessels to the aneurysm.
- Expand the stent to hold the weakened portion of the aorta open, redirecting blood flow through the stent to relieve pressure on the bulging aorta.
After an EVAR, most people recover quickly and can often go home the next day. However, yearly follow-ups with your surgeon are required because the stent can shift over time.
EVAR reduces your hospital stay by 2-3 days and requires less recovery time than traditional open abdominal aortic aneurysm repair.
If EVAR is not an option for you, you may have access to other minimally invasive treatment options. UPMC routinely participates in clinical trials of leading-edge devices to treat complex aortic aneurysms.
Traditional open aneurysm repair surgery
UPMC vascular surgeons are also experts in traditional open aneurysm repair. Your surgeon may recommend this option if your aneurysm does not meet the criteria for an EVAR or if your surgeon believes that you may benefit from an open repair.
In open surgical aneurysm repair, your vascular surgeon will:
- Make a long incision in your abdomen to get to your aorta.
- Remove the weakened portion of your aorta and replace it with a fabric graft.
Because this is a more invasive surgery, your hospital stay will be 5-7 days. Recovery time is six weeks to three months for a complete recovery, depending on your overall health and the extent of your procedure.
How effective is treatment?
Many open aneurysm repairs are successful in the long term with few complications. Follow-up after open aneurysm repair is less frequent than that for EVAR, with most patients coming back every 2-3 years for a checkup.
EVAR requires more frequent follow-up visits and imaging studies to ensure the graft functions properly. You also may require periodic maintenance procedures.
What is the life expectancy of someone with an abdominal aortic aneurysm?
Your life expectancy depends on whether you receive early, effective treatment and the size and extent of your aneurysm. Your doctor will discuss your life expectancy with you.
















