Neuroendoport Clinical Case Study
The Patient
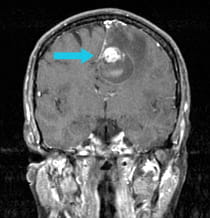
A 52-year-old woman with known breast cancer came to the hospital with progressive right-sided body weakness and a complete inability to speak. An MRI scan showed a metastatic tumor in the deep frontal region with a large amount of edema (swelling and reaction of the surrounding brain).
The Challenge
Because of the weakness and speech problem, there was a great concern regarding the pressure the tumor exerted on the tissue around it. A large opening or brain dissection would risk worsening of her weakness and an inability to recover her speech.
|
Pre-surgical scan shows metastasis on the frontal lobe.
|
|
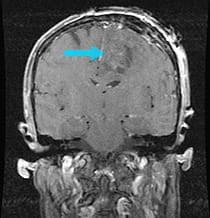
Post-surgical scan shows the successful removal of the tumor following minimally invasive Neuroendoport Surgery.
|
The Solution
The metastatic tumor was removed using the minimally invasive Neuroendoport, and the patient began making words in the recovery room.
The Result
The patient subsequently regained strength in her arm and leg, and her speech eventually returned to nearly normal function over a period of months.
Treatment and results may not be representative of all similar cases.