What Is A Pancreas Transplant?
During a pancreas transplant, a surgeon will place a healthy pancreas from a deceased donor into your abdomen, providing a cure for diabetes. Pancreas transplants are considered for people with diabetes who have severe complications or cannot control their diabetes with other treatments.
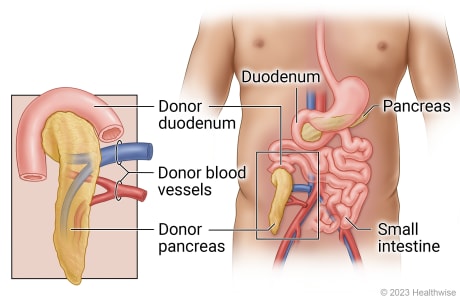
Pancreas transplant
During a pancreas transplant, the diseased pancreas is usually left in place. The donated pancreas is placed in the front part of the belly and connected to the blood vessels of the lower belly. It is connected to your small intestine or your bladder so the digestive juices from the pancreas can drain. A small section of the donor's small intestine (the duodenum) is also transplanted for that purpose.
© 2016-2025 Healthwise, Incorporated. This information does not replace the advice of a doctor.
What are the benefits of a pancreas transplant?
A pancreas transplant often slows down or even reverses secondary complications from diabetes, including eye disease, vascular disease, gastrointestinal problems, and neuropathy.
Types of pancreas transplant
UPMC offers multiple types of pancreas transplants, including:
- Pancreas-after-kidney (PAK) transplant — People who are diabetic after a kidney transplant may receive a pancreas-after-kidney transplant to prevent any future damage to the new kidney. Surgeons transplant the pancreas following a successful kidney transplant.
- Pancreas transplant alone (PTA) — People who have type 1 diabetes with severe, life-threatening complications may be eligible for a pancreas transplant alone.
- Simultaneous pancreas-kidney (SPK) transplant — This type of transplant helps people with type 1 and type 2 diabetes whose kidneys are failing — or have failed — and who need both a new kidney and pancreas. Surgeons transplant both the kidney and pancreas during one surgery.
Conditions we treat with a pancreas transplant
- Diabetes.
- Blood sugar management issues.
- Severe hypoglycemia.
Why Would I Need A Pancreas Transplant?
If you have severe complications related to diabetes, or typical treatments aren’t helping to control your blood sugar levels, you may need a pancreas transplant.
Who’s a candidate for pancreas transplant?
People who are candidates for pancreas transplant include:
- People with type 1 diabetes who have serious complications.
- People with severe hypoglycemia unawareness or severe blood sugar management issues.
- People up to age 55 who are not responsive to other treatments.
- Select individuals with type 2 diabetes.
Patients with type 1 diabetes who have normal kidney function and severe hypoglycemia (Clarke score greater than or equal to 4) usually benefit from a pancreas transplant alone.
Patients with kidney failure referred to our center through their nephrologists are typically candidates for either simultaneous pancreas-kidney or pancreas-after-kidney transplant.
What Are the Risks and Complications of Pancreas Transplant?
Like any surgery, risks associated with a pancreas transplant can include:
- Bleeding.
- Complications related to immunosuppressive medication.
- Infection.
- Organ rejection.
What Should I Expect From Pancreas Transplant?
The first step in the process is for your doctor to refer you to UPMC pancreas transplant services. We also accept self-referrals.
Pancreas transplant patient information review
After the UPMC pancreas transplant team receives your medical records and information listed on the transplant referral checklist:
- A transplant nurse coordinator will collect your medical history, radiology studies, recent blood work, and current physical findings.
- The pancreas transplant team will review the information to determine if a transplant evaluation is appropriate.
- If a transplant evaluation is appropriate, we will obtain insurance authorization and contact you to schedule the evaluation.
Pancreas transplant evaluation
At UPMC, we evaluate patients with severe complications related to diabetes to determine whether they are candidates for pancreas transplant.
Does my care partner need to come to my pancreas transplant evaluation?
We require all candidates to be accompanied by a primary care partner. The evaluation may be physically demanding, and it may be difficult for someone with severe complications from diabetes to get from one appointment/test or location without assistance.
It is also important for the primary care partner to attend the pre-transplant education class, meet with the transplant team members, and learn what to expect as a potential caregiver after the transplant. Being a care partner is a big commitment, and the team will not advocate for listing if a candidate does not have strong care partner support.
Your pancreas transplant evaluation and care team
During your evaluation, you'll have various diagnostic tests and meet with a number of experts from the pancreas transplant team, including:
- Behavioral health nurses or psychiatrists — Will assist you and your family in coping with the stresses associated with chronic disease and the transplant process. They will also assess any current psychiatric/mental health symptoms that are being treated or may need to be treated.
- Credit analysts — Will review your insurance coverage and benefits information. They will help you understand your insurance policy and will be your point of contact for insurance changes. They will also explain any parts of the transplant process that insurance does not cover and suggest options to assist with those costs.
- Endocrinologist — Will examine you, perform a medical history and physical, and focus on the signs and symptoms of your diabetes. They may also review other options for managing your diabetes.
- Gastroenterologist — Diagnoses, treats, and manages pancreas conditions.
- Nutritionists — Will assess your nutritional status, dietary knowledge, and provide education and recommendations for your diet.
- Pancreas transplant nurse coordinator — Will introduce you to the transplant process and review your evaluation schedule. The visit will consist of preliminary health screening, medicine review, and an overview of the transplant process. Your transplant nurse coordinator is here to answer any questions you may have.
- Pancreas transplant surgeons — Will assess your physical capability and risks for transplant. They will review your diabetes management and address all treatment options available to see if a pancreas transplant is the best option for you.
- Pharmacists — Will meet with you to get a complete list of all your medicines and supplements you take, both prescription and over the counter, and ask you how you take your medicines.
- Research transplant coordinators — Transplant nurses who coordinate and oversee patients who participate in research protocols for studies and clinical trials.
- Social workers — Will discuss your support team at home, your prescription insurance coverage, and other social aspects of the transplant process. You will also learn about fundraising options.
Pancreas transplant evaluation testing
Testing will include:
- Blood tests — To determine your blood type and check for signs of disease, infection, or other problems.
- Cardiac (heart) tests— To make sure your heart is healthy before surgery.
- Imaging tests — To assess your abdominal organs and look for signs of other health problems.
After your pancreas transplant evaluation
A multidisciplinary team reviews each patient’s case at a selection meeting and makes decisions regarding approval of pancreas transplant candidates. We will notify you of our decision shortly after the evaluation.
How much does a pancreas transplant cost?
The cost of a pancreas transplant can vary from patient to patient, depending on insurance coverage and other factors. Potential candidates who wish to discuss the estimated costs will be given contact information for patient business services and a transplant credit analyst.
Pancreas transplant waiting list
If you're a candidate for a pancreas transplant, we will place you on the United Network for Organ Sharing (UNOS) waiting list. Prior to being placed on the waiting list, your insurance company has to provide approval. You will be notified regarding the outcome by phone and mail.
If it is determined you are not a candidate for transplant at this time, you may be asked to return for additional testing to be cleared medically to be placed on the waiting list.
Your UPMC pancreas transplant team will continue to manage your diabetes while you wait for an organ with your local medical team.
While on the pancreas transplant waiting list
While on the pancreas transplant wait list, you need to live within a four-hour travel radius of UPMC so you can get to the hospital when we find a pancreas donor match.
You will need to get tests periodically and be seen in the clinic at least every six months so the team can assess your readiness for transplant.
Most patients continue to see their primary endocrinologist for follow-up care during this waiting time. Your doctor will remain in contact with the transplant team at UPMC during this time, in addition to your regularly scheduled visits at UPMC.
If you don't live near Pittsburgh, please find a way to move closer. Family House is an in-between, affordable "home away from home" for pancreas transplant patients and their families. It is not a medical facility.
Learn more about traveling to Pittsburgh for transplant services.
How long will I need to wait for a pancreas transplant?
The average wait time for an SPK is one to two years; for a PAK or PTA, the average wait is two to three years. However, your wait time may vary depending on donor organ availability and other factors.
Your pancreas transplant surgery
Your UPMC transplant coordinator will call you when a donor pancreas becomes available.
Before coming to the hospital
Before coming to UPMC for your pancreas transplant:
- Do not eat or drink anything.
- Take an antimicrobial shower.
- Pack your cell phone and charger.
- Bring all your medications, as well as medications for your care partner, family, and support group.
The surgeon will evaluate the donor pancreas to make sure it is the right size and type and that the antibody panel is a match.
When you arrive at the hospital
When you arrive at UPMC, we will admit you to a patient room where you will:
- Have a history and physical done.
- Have basic testing.
- See an anesthesiologist.
- Sign consent forms for the pancreas transplant surgery.
We will prepare you for pancreas transplant surgery and give you general anesthesia.
How long does pancreas transplant surgery take?
Pancreas transplant surgeries take three to four hours. Combined pancreas-and-kidney transplants take six to eight hours.
During your pancreas transplant surgery
During a pancreas transplant procedure, your surgeon will perform the following steps:
- Make an incision in your abdomen.
- Place the donor pancreas into your abdomen.
- Attach the donor pancreas to your blood vessels and other organs.
- Leave your existing pancreas in place to help with digestion.
- Perform a simultaneous kidney transplant, if required.
- Close the incision.
Your new pancreas should start producing insulin within several hours of your transplant. Your coordinator or surgeon will be able to provide more details about your specific surgery.
Advanced techniques for complex pancreas transplants
UPMC's team of pancreas transplant experts performs many complex pancreas transplant operations. We're equipped to handle the risks of surgery and address any complications.
We also offer “bloodless” surgery for patients who meet strict health requirements. Bloodless medicine means we do not use banked blood products during the operation.
Your recovery after pancreas transplant surgery
Your hospital stay
After pancreas transplant surgery, we will take you to the transplant intensive care unit (ICU), where you will stay for several days.
We will give you pain medicine and antirejection drugs right away.
When your body detects your new pancreas, your immune system begins working to fight what it views as a threat. Antirejection drugs suppress your immune system's natural response to allow your body to accept the new pancreas.
When you're stronger, you will move to a patient room within the transplant unit. You can expect to stay in the hospital for six to eight days.
The pancreas transplant team will monitor your progress to make sure your body isn't rejecting the pancreas and that you aren't developing an infection or other problems.
Going home from the hospital
Before leaving the hospital, your pancreas transplant care team will review your:
- Activity restrictions.
- Blood test schedule.
- Diet and exercise guidelines.
- Follow-up visit schedule.
- Medication schedule.
Be sure you and your care partner fully understand your at-home care plan before you leave the hospital.
You'll also need to care for the incision site to prevent infection. Follow the directions your transplant nurse gave you before leaving the hospital.
Staying close to UPMC
The first few weeks after pancreas transplant surgery are when you have the highest risk for infection or rejection. That's why you will need to remain within one hour of UPMC for at least three to four weeks after discharge or as directed by your transplant team.
You must also have a care partner with you at all times during these first few weeks.
Family House offers a "home away from home" near the hospital until you're ready to return home. It is not a medical facility.
Your care partner's role
An organ recipient needs a lot of help after transplant surgery. Being a care partner is a big responsibility. You may need more than one person to help you for the first few months after your pancreas transplant.
A pancreas transplant care partner will:
- Assist with daily activities within the home.
- Drive you to and from your follow-up appointments.
- Help you record information that the transplant team requests.
- Help you stick to your post-transplant treatment plan.
- Keep family and friends informed of your needs and wishes.
- Look for signs of unusual behavior and contact your transplant coordinator if anything seems wrong.
- Make sure you take medications in the right doses at the right times.
- Provide support, encouragement, and entertainment.
- Run errands, fill prescriptions, and do chores around the house.
- Shop for food and prepare meals.
Your follow-up appointments
At first, you will have frequent follow-up visits so the pancreas transplant team can make sure you're healing properly.
After that, you will return to UPMC's post-transplant clinic at least every few months for the first year.
Our team at UPMC will take care of you for at least the first two years following transplantation, and ideally for life. In some special circumstances, you may be able to find a local transplant center that can take care of you.
Antirejection medications
You'll continue to take the antirejection drugs you received at the hospital for the rest of your life. Your doctor will continuously monitor how you respond and make adjustments as needed to find the right treatment.
The antirejection drugs make you more susceptible to developing infections.
After pancreas transplant surgery, limit your exposure to people with illnesses or places where people are likely to be spreading germs.
Call us if you have any signs of infection, which include:
- Chills.
- Fever over 100.4°.
- Swelling, redness, or fluid draining from the incision site.
Life after pancreas transplant
Most people who receive a pancreas transplant at UPMC have good results and can gradually return to their normal routines within six to eight weeks. You will no longer need to take insulin to manage your diabetes.
To make the most of your new pancreas, it's important to follow your treatment plan and maintain a healthy lifestyle.
Be sure to:
- Take all medications as prescribed — If you have any questions, call our office.
- Stick with your personalized nutrition plan — Follow the recommendations your nutritionist created for you, based on your medications.
- Avoid all nicotine products — This includes cigarettes, cigars, smokeless tobacco, e-cigarettes, nicotine patches, gum, or any other form of pharmaceutical nicotine. You should also avoid all forms of vaping, even if products claim to be nicotine-free.
- Exercise regularly — Begin with short walks, as you're able.
Remember that the UPMC is here for you for the rest of your life.
When to call your doctor about complications
You should let your surgeon know if you have:
- A fever of more than 100.0°F.
- Difficulty breathing.
- Numbness, tingling, pain, swelling, or weakness in your arms or legs.
- Pain, redness, bleeding, drainage, or increased swelling at your surgical site.
- Severe pain that does not respond to medication.
What’s the survival rate after pancreas transplant?
Survival rates for pancreas transplants vary. However, if your pancreas transplant is not successful, you can start taking insulin again and talk to your transplant team about having a second transplant.
Why Choose UPMC for Pancreas Transplant?
When you choose UPMC for pancreas transplant care, you will receive:
- Access to experienced, board-certified specialists — As one of the nation’s most active and experienced transplant programs, UPMC has vast experience in kidney, pancreas, and combined kidney-pancreas transplants.
- Outstanding transplant results — UPMC has extensive experience in pancreas transplant and maintains outcomes comparable to national averages.
- Expert care for complex cases — Our talented team of pancreas transplant surgeons continues to gain vast clinical skills and expertise in the field, allowing them to accept many high-risk patients that other transplant centers may decline.